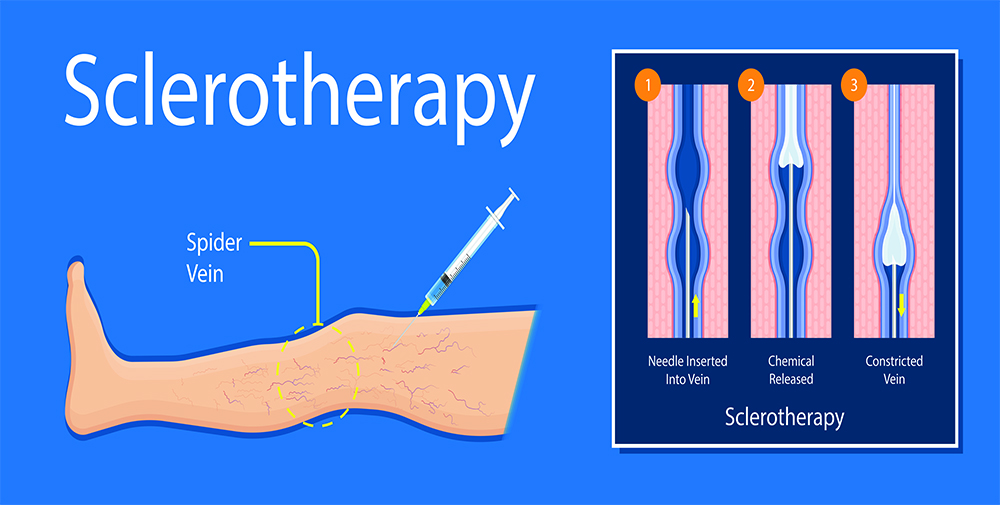
Sclerotherapy is used to treat spider veins and varicose veins by injecting a sclerosing agent into the interior of the troublesome vein. This substance causes the vein walls to become sticky and seal shut. The collapsed vein is reabsorbed into local tissue and eventually disappears. There is little risk of complication, and patients often experience an immediate relief of symptoms.
Light-assisted sclerotherapy is used to treat smaller veins below the skin’s surface. These reticular veins are responsible for feeding the veins that are visible on the surface of the skin. A small, powerful light illuminates the veins and tissue directly below the patient’s skin, allowing the physician to clearly identify the source of the venous dysfunction and to perform the procedure.
Ultrasound-guided sclerotherapy is used for larger, less superficial veins that cannot be seen with transcutaneous illumination (light used to view veins near the surface). Due to proximity of some of these veins to nerves, arteries and other structures, a skilled ultrasound sonographer is critical to the success of this procedure.
After sclerotherapy, treated veins often fade within a few weeks, although it may take longer to see the full results. In some instances, several sclerotherapy treatments may be necessary.
Liquid vs. Foam
There are several kinds of liquid sclerosing agents. The most popular modern sclerosant is call polidocanol. This is a detergent by nature, and therefore, can form bubbles easily. Foam sclerotherapy is, simply put, the mixture of the liquid sclerosant with a gas to create those bubbles.
In the treatment of varicose veins, foaming the sclerosant enables it to displace the blood in larger veins, rather than just mixing with it, as a liquid sclerosant would. That means foam provider a longer contact time between the chemical longer contact time between chemical and the vein wall and is more effective on larger veins, such as the great saphenous vein (GSV) and other truncal veins. Liquid sclerosants work best on the smaller, reticular veins.
Another significant advantage of foam is that it is echogenic, which means that it is easily visible on an ultrasound, increasing the accuracy with which individual veins can be treated.
In addition, because of the efficacy of the sclerosing agent is increased with foam, a lower concentration can be given to treat varicose veins, which means having a smaller total dose of sclerosant to achieve the desired effect.
The most common method for producing foam for sclerotherapy is the “Tessari technique”, which involves manually mixing a small volume of liquid sclerosant with a volume of room air or other gas using two syringes and a three-way tap, or stopcock.
If you or someone you know is suffering from varicose or spider veins, we encourage you to visit our office for a complimentary vein screening. During this screening, we will go over your medical history, complete a visual exam, review your diagnosis and if needed, recommend a venous ultrasound, which will provide the needed results for your treatment options. Please give us a call if you have any questions or would like to schedule your free screenings.
This article was originally published in it’s entirety by Vein Healthcare News and was written by Jennifer Boggs.